DOWNLOAD THIS DOCUMENT IN PDF TO SHARE WITH YOUR FRIENDS & FAMILY
1) Why is it important for me to have the vaccine?
Vaccines activate the body’s immune system to provide specific protection against infections and over the years millions of lives have been saved. With the raging pandemic and the high rate of transmission and severe disease seen with the variants of concern (VOC) it is imperative that we take vaccines to protect not only us but also those around us from COVID-19. Although a higher risk of COVID infections or severe COVID disease has not been definitely proven in AS patients, it appears that certain other rheumatic diseases such as rheumatoid arthritis may indeed increase the risk. More data on risk in AS patients with increasing prevalence of the VOC maybe forthcoming.
2) If you get vaccinated, will you be less likely to get COVID-19?
Yes. The efficacy of the mRNA vaccines is 95% and for the AZ vaccine is 70%. Recently Pfizer updated the numbers based on more data. Efficacy in preventing symptomatic infections was over 90% and 100% against severe infections as defined by the CDC. Even with the very small chance of getting the infection post-vaccine you will be protected against severe disease.
3) What vaccinations are available and is one better than the other?
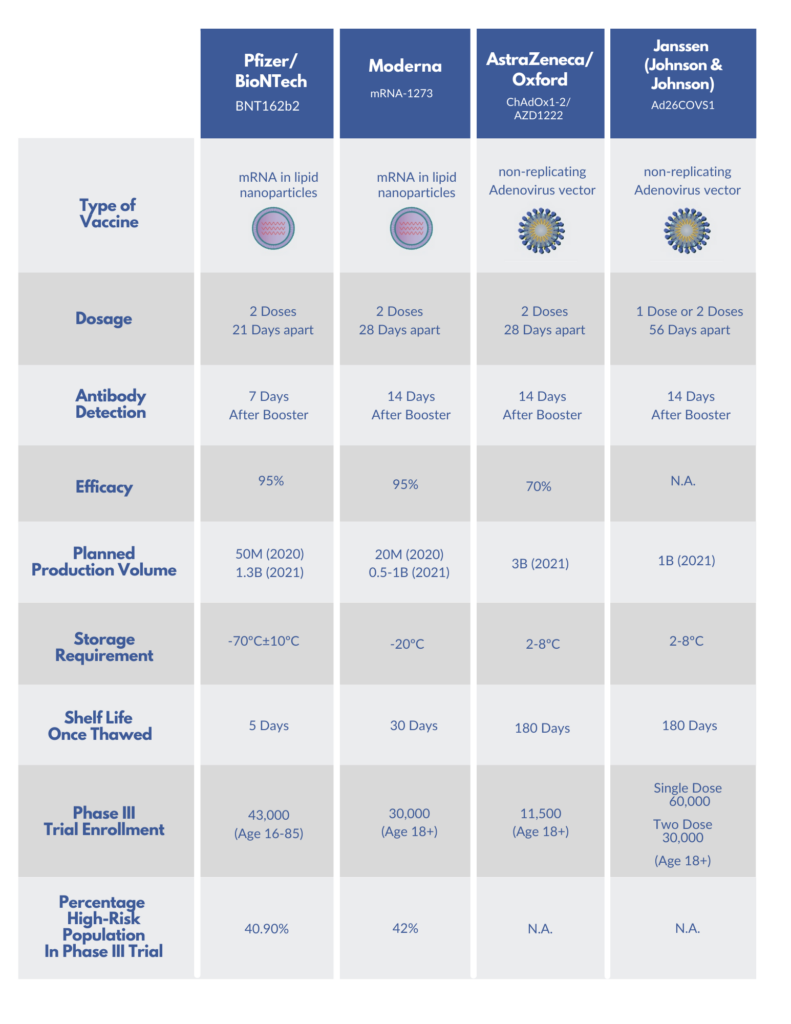
The chance of getting COVID dramatically drops with the decrease in prevalence of the disease in your community. Hence it is important that we all get vaccinated at the earliest. Although the efficacy numbers appear different between the mRNA vaccines and the adenovirus vector vaccines, getting any of the vaccines today will protect us and the community more than waiting for the supply of another vaccine.
4) Do all the vaccinations need a second dose?
Maximal and longer lasting protection is reported after the second dose of the Pfizer, Moderna and AZ vaccines. The J&J vaccine is effective after a single dose.
5) Will the medications I take for my condition affect the way the vaccine works?
Most of the medications used for treating AS have not been shown to decrease vaccine response. Recently a study in patients with inflammatory bowel disease showed decreased response to covid vaccines in those receiving infliximab infusions. For all other TNFi and IL17i used in treating AS, no dose adjustment is recommended. For infliximab although no data on the best way to time the vaccine is not available one may try to take the vaccine mid-cycle between two infusions.
Stopping your treatment puts you at risk for a flare. Everyone in Canada will need to follow Government advice on reducing the spread of Covid-19 even after they have had the vaccine.
6) Should I delay my biologic so that I can have vaccine?
See answer to question 5)
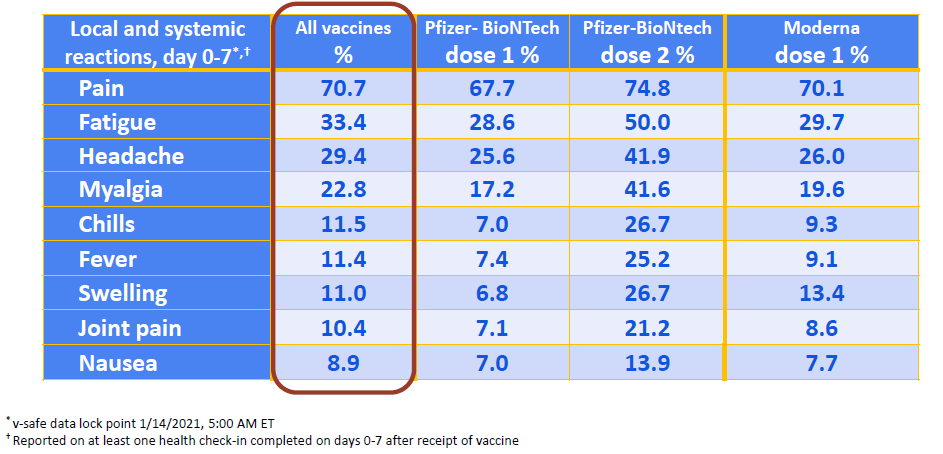
8) Are there side effects?
Please discuss potential adverse events with your family doctor.
7) Can I have the Covid-19 vaccination if I am pregnant or breast feeding?
Follow local guidelines. Although the vaccine has been reported to be safe in pregnant and breastfeeding women, please discuss with your family doctor.
9) How is the vaccine given?
The vaccines are given as an injection in the upper arm.
10) Do you still need to have the vaccine if you have had Covid-19?
Yes, the protection from vaccines may be superior and longer lasting than following natural infection.
For more information on the Covid-19 vaccine rollout in your province, please contact your local health unit.
Contributor: Nigil Haroon, MD, PhD, DM, FRCPC
